Cystectomy and Ileal conduit formation Melbourne
A cystectomy is an operation to remove the bladder. In men, the bladder, prostate, seminal vesicles and lymph nodes are removed. In women, the bladder urethral, part of the vagina and lymph nodes are removed. In addition, the uterus, fallopian tubes and ovaries may be removed.
An ileal conduit is the redirection of the urine so that it drains into a bag located on the right side of your abdomen. This diversion is created by removing a small section of the small bowel (ileum) which is used as a conduit to allow urine to flow out. The ureters will be surgically sewn to the wall of the conduit. The surgeon will close one end of the conduit and will bring the open end through the abdominal wall creating a stoma. The stoma is composed of mucous membrane of the intestine.
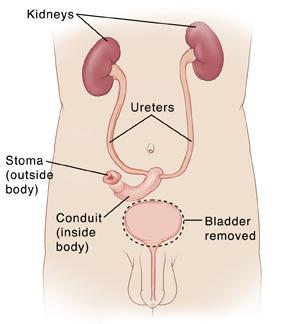
Before surgery
- Ensure your hospital paperwork is completed and sent to the hospital at least 7 days before surgery.
- Ensure you have all your tests completed 4-7 days before surgery. These include bloods, ECG and urine test.
- You will be admitted the day before surgery approximately 2PM to enable commencement of bowel preparation at 4PM. You will also commence clear fluids on admission.
- You will be seen by the Stomal Therapist for siting of a stoma.
- Once admitted, you will be issued with anti-embolic stockings (compression stockings). You are required to wear these throughout your admission.
- If you are a Diabetic, please speak to the Practice Nurse at your earliest convenience.
- If you are on any blood thinning medications, then please alert the nurse at your earliest convenience.
- Please inform staff if you have any allergies.
You will remain in hospital 10-14 days. Before discharge, you will be taught how to look after your stoma. You will be given adequate supplies and be asked to join the Ostomy Association. The Stomal therapy nurse will explain this to you.
Following surgery and whilst in hospital
- You will be admitted to HDU for 1-2 days.
- You will have intravenous fluids via a central line until you are drinking fluids
- You will remain on nil orally until bowel sounds return. This may take 5-6 days.
- Your stoma will be monitored carefully by nursing staff throughout your admission. The stomal therapist will also see you to begin your education. This will occur towards the end of your admission.
- As bowel sounds return, you will be commenced on sips of water. If you are tolerating this, you will then progress slowly to free fluids and then light diet and full ward diet (usually by day 7). Your central line will then be removed.
- You drain tube will be removed by nursing staff once drainage has stopped and following permission by the surgeon (this usually occurs around day 5 following surgery).
- Your wound dressing will be monitored by nursing staff and dressings will be attended as required.
- You will have two stents in-situ which can be seen through the stoma bag (They help with the flow of urine while the surrounding tissue heals). These will be removed just before discharged or you will return to the rooms to have these removed 3 weeks following surgery.
- Following surgery, the stoma may be swollen and may take several months for it to shrink to it is permanent size. The stoma is not painful as it does not contain any nerve endings.
- You will be discharged when you are eating and drinking well and you’re able to look after your stoma.
Following discharge
- It is normal to feel tired following surgery. It is important you get plenty of rest, eat a well-balanced diet and do gentle exercises such a walking. Avoid stairs if possible.
- Ensure your bowels are regular. A high fibre diet with adequate fluids is essential. Avoid constipation as this may cause discomfort. Speak to the Practice Nurse for further advice.
- Take regular pain relief as required. Avoid codeine as this may cause constipation.
- Your wound dressing will be removed before discharge. Your sutures are dissolvable and therefore will dissolve within 1-2 weeks. Please call the rooms if you notice redness, swelling and or discharge from the wound.
- It is important you drink adequate fluids and to ensure your urine is pale yellow during the day.
- You are advised to avoid heavy lifting for 6 weeks and any strenuous exercise or activities for 6 weeks. Strenuous exercise includes bike riding, running, horse ring and golf. Avoid stairs for the first few weeks.
- Drink 2 litres of fluid per day to ensure your urine is pale yellow and to help flush out your bladder.
- Return to work is dependent on the type of work you do. Generally being off work for 6 weeks is recommended. If you wish to return earlier you will need to discuss this with your surgeon.
- No driving is allowed for 6 weeks.
- You are required to return to the rooms for your first appointment following surgery approximately 1 week following discharge to have your stents removed (if this wasn’t done before discharge). You are then required to have a review appointment approximately 4 weeks later. Please call the rooms if this appointment was not made for you.
You must contact the rooms if you experience any of the following:
- Redness, swelling and presence of purulent discharge from the wound
- Fever, chills, sweats
- Cloudy, offensive urine
- Decreased or no urine output
- Loss of appetite
- Swelling and redness in your legs
- Shortness of breath/back pain
- Severe abdominal, back or flank pain
- Stoma – red, inflamed and draining pus


